- SUMMARY
- Eczema
Eczema
- Living with eczema day to day
- Eczema: what foods should you eat?
- Eczema: how can flare-ups be avoided?
- Eczema cream, ointment: what should you use?
- What soap should be used for eczema?
- Swimming pool, swimming when you have eczema?
- Eczema: What daily reflexes should you adopt?
- Which detergent should eczema patients use?
- What are the habits to avoid when you have eczema?
- Eczema: can it be cured?
- Eczema: how to treat itching
- What causes eczema?
- Perspiration-induced eczema
- Contact eczema due to nickel and chromium
- Hereditary eczema
- Contact eczema due to cosmetics
- Allergy-induced eczema
- Contact eczema due to medication and topical treatments
- Contact eczema due to cleaning products
- Stress-induced eczema
- Clothing contact eczema
- Body eczema: hands, feet, arms, back, face, etc.
- Scalp eczema
- Leg eczema or varicose eczema
- Eczema around the mouth
- Hand and finger eczema (chronic hand eczema)
- Eczema in the ears
- Foot eczema
- Eczema on the neck and nape of the neck
- Facial eczema
- Arm eczema (elbows, armpits, forearms)
- Eczema on the stomach and belly button
- Eczema of the eyelids, eyes or palpebral eczema
- Eczema on the back
- What is infantile eczema?
- Eczema in babies: what habits should you adopt?
- Eczema in babies and children: the areas most often affected
- What soap should be used for babies with eczema?
- When should you consult a physician about your baby's eczema?
- Cortisone cream to relieve eczema?
- How should you treat baby’s and infant’s eczema?

Eczema
Updated on , validated by the medical directorate.
Eczema is a skin disease that can occur at any age. Since it is a very common condition, (affecting approximately 20% of children and 3 to 4% of adults) and relatively benign, the general public tend to downplay the seriousness of eczema. At the same time, there are many misconceptions surrounding the issue. Do you or one your close friends or family have eczema? If so, you'll know that eczema is a disease in its own right that can often cause physical and psychological damage. Would you like some precise and detailed information about eczema? You’re in the right place!

What you should know about eczema?
Eczema is a dermatosis, or skin disease, that is both chronic and inflammatory. It alternates between active periods known as flare-ups and periods of remission with no (or very few) symptoms.
However, this is only a general definition, as there are several types of eczema. The most well-known form is atopic eczema which mainly affects very young children.
In adults, eczema can manifest in numerous forms: localized outbreak on the face and neck, hand eczema, generalized eczema, etc. More often than not, the condition has been present since childhood but it can also occur suddenly in adults. In pregnant women, it is impossible to predict in advance if eczema will improve, or conversely, be aggravated during pregnancy.
Some of the other most common forms of eczema are: contact eczema, where lesions appear specifically after prolonged contact with an allergenic substance, and chronic hand eczema, which is most commonly caused and/or aggravated by irritants, especially in the workplace.
In all cases, rest assured: eczema is not contagious.
What are the causes of eczema?
Everyone with eczema dreams about it: finding a single unique cause responsible for their lesions. However, the reality is often very different, with not one but several causes of eczema.
Stress is often blamed but it is not systematically responsible, quite simply because eczema is not a psychosomatic disorder (meaning it does not result from the mind affecting the body). Unfortunately, far too often, people can be heard saying "eczema, it's all in the head". Eczema is not in the head but on the skin!
Perspiration can cause certain flare-ups and this requires implementation of preventive measures, for example, when playing sport.
Eczema can be linked to allergies. This is especially the case with contact eczema, although the substance responsible is often difficult to identify. The allergen is sometimes hidden in everyday objects: in a piece of clothing, an accessory, a piece of jewelry or a cosmetic. In atopic eczema, the allergy is often less specific and closer to a heightened sensitivity. It is determined genetically rather than being an allergy in the true sense. Heredity plays a major role in atopic eczema.

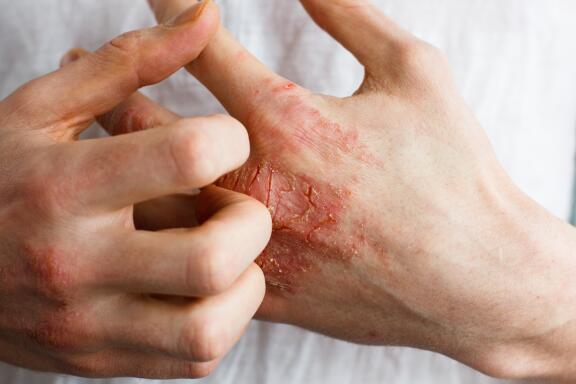
Symptoms of an eczema flare-up
An eczema flare-up is characterized by red plaques which are not clearly defined, meaning the edges are not distinct. The plaques can alternate between being swollen and oozing, or conversely, dry and rough. Skin affected by eczema is sore, it stings, it burns, and mainly it itches. Itching is a recurring symptom of eczema. When people have eczema, it is often difficult for them to remember not to scratch and aggravate the situation. Another major symptom of eczema is skin dryness, especially in the case of atopic eczema. This dryness can spread from head to toe, even in areas other than the eczema plaques.
The various treatments prescribed by the physician will help control the symptoms and improve the condition of the skin.
Diagnosis : you have plaques, dandruff, redness, itching ?
Do you have any of the following symptoms in your scalp and/or face and body?
- plaques
- dandruff
- redness
- itching
Wonder what it is?
It could be psoriasis, seborrheic dermatitis, or even eczema.
Make the diagnosis "Plaques, dandruff, redness and/or itching?" to discover our advice and recommendations for adapted care routines.


What is infantile eczema?
Eczema can occur in the first few months of life. Before the age of 2, eczema mainly affects the outside of the limbs, the torso and the cheeks. After age 2, the condition mainly affects the skin folds: neck, elbows, knees, wrists, ankles, etc.
In cases of infantile eczema, a physician should be consulted to make an official diagnosis and prescribe suitable treatment. The physician and afterward the pharmacist are there to help the family fully understand and integrate the treatment into their daily life.
Cleansing is also a major factor in treatment. Patients with eczema should preferably take quick showers, in warm water, and using a cleansing product specifically for atopic skin.
Living with eczema day to day
Living with eczema day to day is not always easy. A few simple habits can improve the condition of the skin and, at the same time, quality of life. For example, various tips enable you to reduce itching: they are predominantly based on cold treatments but can also involve keeping hands busy, for example, with a foam ball. It is important to avoid scratching to reduce the risk of secondary infection and scarring.
Taking care of your skin, i.e. with gentle cleansing and then moisturizing, must become a daily reflex. Adapting the environment should not involve setting very strict or expensive rules, instead it should rely on common sense: vacuum regularly, wear clothes made from natural fibers, opt for a hypoallergenic detergent and limit the use of softeners.
Some questions crop up again and again, especially in relation to food. It is true that some cases of eczema are linked to food allergies, however this must not lead to patients adopting highly restrictive diets because there is a risk of nutritional deficiencies, particularly in growing children.
Medicinal treatment and following simple steps for healthy living can limit the number of flare-ups and improve quality of life.

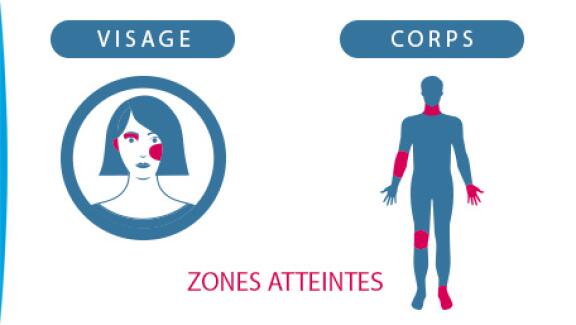
Areas affected by eczema
Eczema can affect all areas of the body. Eczema on the stomach can develop in the first few months of life and will often spread over the whole area. It can also occur on localized areas, such as the belly button.
When on the arms, eczema occurs on the outer sides and curved parts, or conversely in the skin folds, such as the elbow and wrist folds.
Other areas, such as the back, foot or leg may be affected by eczema. Although the plaques are less noticeable in these areas, itching and discomfort are still present.
In the case of eyelid eczema, or palpebral eczema, and hand eczema, the affected area is very small but particularly noticeable and difficult to live with on a daily basis.
Eczema commonly affects the face and neck, especially in adults. This causes a great deal of embarrassment, and sometimes it's difficult to cope with other people staring. The nape of the neck and ears can also be affected. Eczema around the mouth is very common in both children and adults.
Finally, scalp eczema should be checked for an associated pathology, such as seborrheic dermatitis or psoriasis
Childhood eczema
Eczema affects one in five children and is therefore very common. Childhood eczema is almost always atopic dermatitis, which is a constitutional eczema marked by dry, porous skin that quickly becomes inflamed after contact with environmental allergens.
Most of the time, children with eczema scratch and sleep poorly. Treatments with cortisone creams and emollients usually stop flare-ups within a few days, although children must be willing to apply them! To encourage children's compliance, parents can, for example, suggest applying the cream while listening to music.
What is the best treatment for eczema?
In most cases, eczema treatment is based on topical corticosteroids for inflammatory flare-ups and long-lasting emollients to strengthen and protect the skin. Other treatments exist in the form of creams, tablets, injections; they are prescribed on a case-by-case basis by the dermatologist. In the case of contact eczema, the removal of the substance is essential if the eczema is to be stopped.
The various treatments for eczema do not cure the disease, but they can limit the appearance of flare-ups and reduce symptoms, especially itching. Eczema can also eventually disappear on its own, for example, as a child grows older. In the meantime, you have to learn to "live with it" in some way, and that is certainly the most difficult part of managing it.
Occupational dermatoses
As its name suggests, an occupational dermatosis is a skin disease that develops in the workplace. Most often, it is an occupational eczema mainly located on the hands. Occupational dermatosis then results in the appearance of red, rough and itchy plaques.
All sectors are concerned by occupational eczema: hairdressing, beauty care, construction and public works, hospitals, etc. The management of an occupational dermatosis is based both on curative measures using cortisone creams, and preventive measures to avoid the development of eczema: wearing gloves, application of an insulating barrier cream, etc.
The application that helps you live better with eczema
The Pierre Fabre Eczema Foundation has developed ECZEMA CARE+, an application to help you manage your eczema.
As a patient, ECZEMA CARE+ helps you to better follow the evolution of your disease, and to share your information and feelings with your healthcare team. You’ll also have access to a wealth of practical advice and tools to help you better understand your condition and live with it on a daily basis.
The DUCRAY Dermatological Laboratories support the Pierre Fabre Eczema Foundation.

Playing YouTube videos requires the use of cookies in order to offer you targeted advertising based on your browsing For more information, please visit YouTube's « cookie » policy.
You have rejected Youtube's cookies and therefore you cannot view the video.
You can change your choices by clicking on « Cookie Settings » and accept Youtube's cookies to enable the video.
You can change this setting and withdraw your consent at any time.
Our care routines
Skin prone to atopic eczema, contact eczema, chronic eczema and/or, eyelid eczema
- Discover Eyelid atopic-prone skin
Eyelid atopic-prone skin
- Discover Atopic-prone skin on the face and body
Atopic-prone skin on the face and body
- Discover Chronic atopy on hands
Chronic atopy on hands
- Discover Anti-scratching body
Anti-scratching body
Dermatological expertise
To better understand your skin and hair, discover our exclusive content and innovative care products designed to improve your quality of life..
